Search
- Page Path
- HOME > Search
Original Articles
- Thyroid
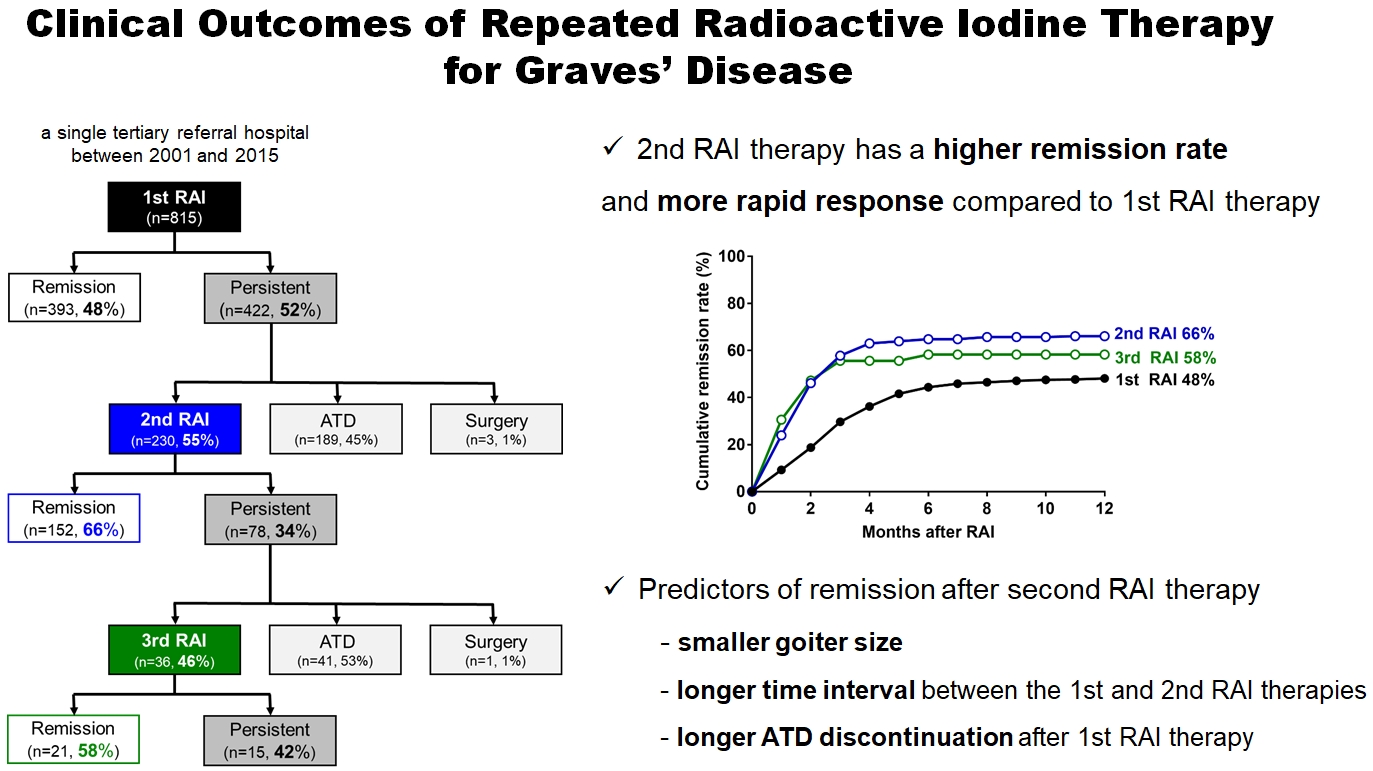
- Clinical Outcomes of Repeated Radioactive Iodine Therapy for Graves’ Disease
- Min Joo Kim, Sun Wook Cho, Ye An Kim, Hoon Sung Choi, Young Joo Park, Do Joon Park, Bo Youn Cho
- Endocrinol Metab. 2022;37(3):524-532. Published online June 16, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1418
- 4,872 View
- 231 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Radioactive iodine (RAI) therapy is a successful therapeutic modality for Graves’ disease. However, RAI therapy can fail, and RAI therapy after antithyroid drugs (ATDs) has a lower remission rate. Therefore, many patients require repeated RAI therapy. This study investigated the clinical outcomes of repeated RAI therapy for Graves’ disease.
Methods
Patients who underwent RAI therapy as second-line therapy after failure of ATD treatment between 2001 and 2015 were reviewed. Remission was defined as hypothyroid or euthyroid status without ATD, and with or without levothyroxine at 12 months after RAI therapy.
Results
The 1-year remission rate after 2nd RAI therapy (66%, 152/230) is significantly higher than that after 1st RAI therapy (48%, 393/815) or long-term ATD treatment after 1st RAI therapy failure (42%). The clinical response to 2nd RAI therapy was more rapid. The median time intervals from the 2nd RAI therapy to ATD discontinuation (1.3 months) and to the start of levothyroxine replacement (2.5 months) were significantly shorter than those for the 1st RAI therapy. A smaller goiter size, a longer time interval between the 1st and 2nd RAI therapies, and a longer ATD discontinuation period predicted remission after the 2nd RAI therapy. Finally, in 78 patients who failed the 2nd RAI therapy, the mean ATD dosage significantly reduced 5.1 mg over 12 months.
Conclusion
Repeated RAI therapy can be a good therapeutic option, especially in patients with smaller goiters and those who are more responsive to the 1st RAI therapy. -
Citations
Citations to this article as recorded by- The Early Changes in Thyroid-Stimulating Immunoglobulin Bioassay over Anti-Thyroid Drug Treatment Could Predict Prognosis of Graves’ Disease
Jin Yu, Han-Sang Baek, Chaiho Jeong, Kwanhoon Jo, Jeongmin Lee, Jeonghoon Ha, Min Hee Kim, Jungmin Lee, Dong-Jun Lim
Endocrinology and Metabolism.2023; 38(3): 338. CrossRef - Effect of liver dysfunction on outcome of radioactive iodine therapy for Graves’ disease
Yuyang Ze, Fei Shao, Xuefeng Feng, Shanmei Shen, Yan Bi, Dalong Zhu, Xiaowen Zhang
BMC Endocrine Disorders.2022;[Epub] CrossRef
- The Early Changes in Thyroid-Stimulating Immunoglobulin Bioassay over Anti-Thyroid Drug Treatment Could Predict Prognosis of Graves’ Disease

- The Localization of Microadenoma with Sella Imaging Study and Inferior Petrosal Sinus Sampling in Cushing's Disease.
- Jae Seok Jeon, Sang Jeon Choi, Chan Soo Shin, Kyoung Soo Park, Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee, Chang Soon Koh, Hee Won Jung, Dae Hee Han, Moon Hee Han, Kee Hyun Chang
- J Korean Endocr Soc. 1996;11(4):492-499. Published online November 7, 2019
- 1,016 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Inferior petrosal sinus sampling(IPSS) is known to be useful for the differential diagnosis of ACTH-dependent Cushings syndrome and for the preoperative lateralization of pituitary microadenoma. We tried to analyze the relative value of IPSS in localization of microadenoma as compared with sella imaging study including computerized tomogram(CT) or magnet resonance imaging(MRI) in Cushings disease. Methods: We reviewed the clinical records of 21 patients with Cushings disease who underwent IPSS and the radiologic study such as sella CT or sella MRI preoperatively followed by transsphenoidal microsurgery. By pathologic examination including immunohistochemistry and postoperative clinical and biochemical evaluation we confirmed the diagnosis of Cushings disease due to pituitary microadenoma in all 21 cases. Results: Sella CT or sella MRI detected microadenoma in 57.1% of cases( =12/21), while recently available dynamic MRI did so in 7 out of S cases. With IPSS the diagnosis of Cushings disease was possible in 90.5% of cases(= 19/21), but accurate lateralization of microadenoma was achieved in only 63.2% of cases( =12/19). IPSS precisely localized the pituitary microadenoma in 6 out of 9 cases whose lesion were not detected by the radiologic study. Of 7 cases in which IPSS failed to localize microadenoma, the radiologic study detected the lesion in 6 cases. Of 5 cases in which IPSS and the radiologic study showed a discrepancy in location of microadenoma, the radiologic study correctly localizaed the lesion in 4 cases and IPSS did so in one case. Conclusion: IPSS is not more reliable than sella imaging study for preoperative localization of microadenoma in Cushings disease. However it might have a complementary role, especially when sella imaging study failed to visualize the lesion.

- The Incidence of Thyroid Autoantibody in Subacute Thyroiditis and the Clinical Characteristics of Greeping Thyroiditis.
- Jae Seok Jeon, Won Bae Kim, Hae Young Park, Young Joo Park, Hyun Kyung Chung, Sang Jeon Choi, Chan Soo Shin, Kyoung Soo Park, Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee, Chang Soon Koh
- J Korean Endocr Soc. 1996;11(4):438-446. Published online November 7, 2019
- 1,264 View
- 30 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Subacute thyroiditis is a spontaneously resolving inflammatory disorder of thyroid gland, usually associated with painful goiter and short-lived thyrotoxicosis. Although its etiology is yet to be established, much evidence suggests viral infections and genetic factors play important roles. Usually, both lobes of thyroid gland are involved simultaneously, but in some patients one lobe is involved first and the other later(creeping thyroiditis), Thyroid autoantibodies which might appear probably due to inflammatory release of thyroid antigens, are found in a variable number of patients with subacute thyroiditis. However there have been few detailed reports on their incidence in Korean patients with subacute thyroiditis. So, we were to see the elinical characteristics of patients with subacute thyroiditis with special regards to the incidence of thyroid autoantibodies and to the incidence and characteristics of creeping thyroiditis, Methods: We reviewed the clinical records of 85 patients with subacute thyroiditis(7 men and 78 wornen, meam age of 43+9 years) who had visited the thyroid clinic in Seoul National University Hospital between 1986 and 1994. Results: At initial visit, the incidenees of thyroid autoantibodies were as follows: anti- microsomal antibody 7.8%, anti-thyroglobulin antibody 22.1%, and thyratropin binding inhibitor inununglobulin 6.3%. During the follow-up period, thyroid autoantibodies appeared most frequently between the first and the second month after initial visit. Compared to those with non-creeping thyroiditis, the patients with creeping thyroiditis(21.4%) had nonspecific systemic sy~rnptoms more frequently(89% vs. 42%, p<0.05). They required steroid therapy more ftequently(89% vs. 52%, p <0.05), and needed longer duration of treatment(9.3+6.2weeks vs, 4.7+3.7weeks, p<0.05). The incidence of abnormalities in liver function and the incidence of thyroid autoantibodies were higher in non-creeping thyroiditis group. Conclusion: In accordance with previous reports, thyroid autoantibodies were detected in only a small portion of Korean patients with subacute thyroiditis. Rather different clinical manifestations and different incidences of thyroid autoantibodies between ereeping group and non-creeping group suggest differences in the pathogenetic mechanisms between those two groups. However, there is need for further study to validate such observation and to elucidate the mechanisms.

- A Clinical Study on Hypopitutiarism: Significance of Combined Pituitary Stimulation Test.
- Bo Youn Cho, Hong Gyu Lee, Chang Soon Koh, Hyung Kyu Park, Sook Kyung Kim, Chan Soo Shin, Seong Yeon Kim, Jae Seok Chun, Kyung Soo Park, Hyeon Kyu Kim, Sun Wook Kim
- J Korean Endocr Soc. 1996;11(3):268-276. Published online November 7, 2019
- 1,237 View
- 25 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Hypopituitarism can be caused by various diseases. Its clinical manifestations vary, depending on the extent and severity of the pituitary hormone deficiency. And some patients may initially present with SIADH-like features. Combined pituitary stimulation test has been used for the diagnosis of hypopituitarism and subsequent hormone replacement therapy. However, the test is laborious, expensive and uncomfortable to the patients, So we performed this study to know whether combined pituitary stimulation test can be replaced with clinical features and simple basal hormone concentrations. Methods: Fifty-four patients who were diagnosed as hypopituitarism by combined pituitary stimulation test were included in this study. Clinical features and basal hormone data were compared with the results of combined pituitary stimulation test for the evaluation of pituitary-gonadal, pituitary-thyroid, and pituitary-adrenal axes, using X2 test. Results: 1) In pituitary-gonadal axis, the evaluation of clinical features and basal gonad hormone concentrations were significantly consistent with stimulation test(p<0.05), 2) In pituitary-thyroid axis, the evaluation of basal thyroid hormone concentrations were more helpful than stimulation test though results of the two tests were not consistent. 3) In pituitary-adrenal axis, all patients whose basal cortisol concentrations were low showed inadequate responses to stimulation test. However, stimulation test revealed adrenal insufficiency in some patients with normal basal cortisol concentrations. 4) 9 patients who presented with SIADH-like features were older than the others and had all corticotropin deficiency. Conclusion: In patients with suspected hypopituitarism, the evaluation of clinical features and basal hormone concentrations can be sufficient for the diagnosis of hypopituitarism and hormone replacement therapy. However, stimulation test is necessary to investigate adrenal function in patients with normal basal cortisol concentrations. And hypopituitarism should be considered in old patients who present with SIADH-like features.

Case Report
- A Case of Symptomatic Severe Hypercalcemia as Initial Manifestation of Hyperthyroidism.
- Hye Young Park, Won Bae Kim, Hyeon Kyu Kim, Chan Soo Shin, Seong Yeon Kim, Bo Youn Cho, Hong Gyu Lee, Chang Soon Koh
- J Korean Endocr Soc. 1996;11(1):124-126. Published online November 7, 2019
- 1,108 View
- 20 Download

Original Articles
- Clinical Characteristics of Graves' Disease Patients with Undetectable Thyrotropin Binding Inhibitor Immunoglubulin (TB2).
- Bo Youn Cho, Won Bae Kim, Hong Gyu Lee, Chang Soon Koh, Seong Yeon Kim, Seok In Lee, Jae Seok Chun, Kyung Soo Park
- J Korean Endocr Soc. 1996;11(1):68-74. Published online November 7, 2019
- 1,612 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Graves disease is an autoimmune disease caused by TSH receptor antibodies. Thyrotropin binding inhibitor immunoglobulins(TBII) are detected in most Graves patients, but some patients have no TBII activities in their sera. It is unknown whether the clinical features of TBII-positive patients are different from those of TBII-negative patients. Methods: To evaluate the prevalence of TBII-negative Graves' patients and its clinical differences from TBII-positive patients, we examined TBII by radioreceptor assay in 686 consecutive untreated Graves patients. We found 84 TBII-negative patients(15 men and 69 women, mean age ±EM: 40.9±.4 years) and compared their clinical characteristics with 87 TBII-positive patients (22 men and 65 women, mean age±EM: 39.9±.5 years) who were selected randomly from the same patients group. Results: In this study, TBII was undetectable in 12.2% of patients with Graves' disease(84 of 686). TBII-negative group had a less weight loss than TBII-positive group. However, there was no significant differences in age, sex ratio, prevalence of ophthalmopathy, duration of illness and positive rate of family history for thyroid diseases between TBII-negative and -positive groups. Serum total T or T levels were not different from each other, but T3-uptake was significantly higher in TBII-positive group than that in TBII-negative group, suggesting that the free hormone levels in TBII-negative group might be lower. The thyroid uptake of 99mTcO4 was significantly higher in TBII positive group than that in TBII-negative group. Thyroid autoantibodies, including antimicrosomal and antithyroglobulin antibodies were detected in almost all patients but there were no differences in titers and positive rate between TBII-negative and -positive groups. Conclusion: Although TBII-negative Graves patients showed less weight loss and low 99mTc04 thyroidal uptake compare to TBII-positive patients, the clinical and immunological characteristics of TBII-negative patients are not different from TBII-positive one.

- Changes in Serum Lipids and Apolipoproteins Levels According to the Thyroxine Treatment in The Patients with Subclinical Hypothyroidism.
- Hye Young Park, Bo Youn Cho, Won Bae Kim, Hong Gyu Lee, Chang Soon Koh, Geon Sang Park, Hyung Kyu Park, Sook Kyung Kim, Chan Soo Shin, Seong Yeon Kim
- J Korean Endocr Soc. 1996;11(1):41-51. Published online November 7, 2019
- 1,221 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Subclinical hypothyroidism(SCH) is a common biochemical abnormality which can be found in routine screening tests of thyroid function. We are increasingly faced with the question of whether its an indication for thyroxine replacement therapy. The effect of thyroxine replacement on lipid profile in SCH has aroused a great interest because of an association of overt hypothyroidism(OVH) with hyperlipidemia and increased risk of coronary artery disease. Method: We prospectively evaluated the changes in lipids and apoproteins before and after thyroxine replacement therapy in 23 patients with SCH and in 37 patients with OVH. We measured serum total cholesterol and triglyceride using autoanalyzer, high density lipoprotein(HDL) chole-sterol by dextran sulfate method, Apo A1 and Apo B by immunonephelometric assay. Results: Thyroxine replacement therapy significantly decreased total cholesterol, low density lipoprotein(LDL) cholesterol and apo B levels, but did not affect the level of triglyceride, HDL cholesterol or apo AI in patients with OVH. In SCH, thyroxine replacement therapy with the doses to normalize serum TSH concentrations also decreased significantly the level of cholesterol and LDL cholesterol albeit apo B levels did not change. Moreover, in most of patients with OVH (11 of 12) and in all of patients with SCH(5 of 5) who had had hyperchlesterolemia before treatment, thyroxine replament normalized their cholesterol and LDL cholesterol levels. Conclusion: In regard to the beneficial changes in blood lipid levels, patients with SCH should be treated, especially in cases who have other risk factors for the development of atherosclerosis. If thyroxine replacement only will reduce the incidence of coronary artery disease in SCH remains to be elucidated by long-term prospective studies.

- Spontaneous Recovery from Hypothyroidism in Autommune Thyroiditis.
- Bo Youn Cho, Jae Hoon Chung, Kwang Won Kim, Kyu Jeung Ahn, Yong Ki Min, Myung Shik Lee, Moon Kyu Lee
- J Korean Endocr Soc. 1996;11(1):30-40. Published online November 7, 2019
- 2,194 View
- 34 Download
-
 Abstract
Abstract
 PDF
PDF - Background
A lifelong thyroxine therapy is indicated in all patients who have hypothyroidism as a result of autoimmune thyroiditis. However, it has been reported that some hypothyroid patients with autoimmune thyroiditis have spontaneous remission with restriction of iodine intake instead of thyroxine therapy. The purpose of study was to investigate how many hypothyroid patients with autoimmune thyroiditis can recover from hypothyroidism with restriction of iodine intake instead of thyroxine therapy and which factors predict recovery from hypothyroidism. Methods: We studied 64 patients with autoimmune thyroiditis(goitrous autoimmune thyroiditis 56, atrophic autoimmune thyroiditis 8). Thyroxine therapy was discontinued in patients with goitrous autoimmune thyroiditis on the way(group 1, n=32) or from the beginning(group 2, n=24) and atrophic autoimmune thyroiditis on the way(group 3, n-8). All patients were asked to avoid iodine-rich foods and thyroid function was monitored every one to two months for up to 35 months. Serum T3, T4, TSH concentrations, antithyroglobulin and antimicrosomal antibodies were measured by radioimmunoassay(RIA). TSH binding inhibitor immunoglobulin(TBII) was measured in serum using radioreceptor assay. Two hundred micrograms of thyrotropin releasing hormone (TRH) were given as intravenous bolus and TSH levels were measured in blood samples taken at 0, 30, and 60 minutes. All values were expressed as mean+-SEM. Statistical analysis was done with paired or non-paired t-test, ANOVA, and the Chi-square test. Statistical significance was defined as p-value below 0.05. Results: Thirteen(40.6%) of 32 patients in group 1 remained euthyroid after 12-35 months of discontinuation of thyroxine therapy. The other 19(59.4%) patients in group 1 had recurrences of hypothyroidism within 3 months after discontinuation of thyroxine therapy. In 11(45.8%) out of 24 patients in group 2, serum TSH concentrations declined below 5 mU/L within 3 months without thyroxine therapy. The other 13(54.2%) patients in group 2 remained hypothyroid till 2-16 months and the thyroxine was given. In contrast, all 8 patients in group 3 had recurrences of hypothy- roidism within 3 months after stopping thyroxine therapy. When we compared the recovered patients of goitrous autoimmune thyroiditis with the non-recovered patients of goitrous autoimmune thyroiditis, regardless of thyroxine therapy from the beginning, age at onset of disease of the 24 recovered patients was significantly younger than the 32 non-recovered patients(30.1+2.0 years vs. 40.2+ 2.4 years; p=0.004). Concl#usion: These findings suggest that 42.9% of hypothyroid patients with goitrous autoim- mune thyroiditis remain or become spontaneously euthyroid with restriction of iodine intake instead of thyroxine therapy. Young age may be a predicting factor of recovery from hypothyroidism in goitrous autoimmune thyroiditis.

- Difference of Thyroid Stimulating Antidody Activities Measured in Chinese Hamster Ovary Cells Stably Transfected with Human TSH Receptor and in FRTL-5 Cells in Graves Disease and Its Clinical Correlations.
- Young Kee Shong Young Kee Shong, Hye Young Park, Bo Youn Cho, Won Bae Kim, Hong Gyu Lee, Chang Soon Koh, Yeon Sang Oh
- J Korean Endocr Soc. 1996;11(1):18-29. Published online November 7, 2019
- 1,111 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Background
: Thyroid stimulating antibodies result in the development of hyperthyroidism and goiter in Graves disease. However, thyroid stimulating antibody activities do not correlate with the clinical features in many patients with Graves disease. The purpose of this study is to address this discrepancy between thyroid stimulating antibody activities and clinical features of Graves patients. Methods: We measured thyroid stimulating antibody activities simultaneously using human TSH receptor transfected Chinese hamster(hTSHR-CHO) cells and rat thyroid(FRTL-5) cells in 57 untreated patients with Graves disease, and compared their activities with clinical features including thyroid hormone levels. Results : The detection rate of thyroid stimulating antibody measured by hTSHR-CHO cells was 90% in 57 untreated Graves patients and it was higher than that measured by FRTL-5 cells. Thyroid stimulating antibody activity by hTSHR-CHO cells was significantly correlated with that by FRTL-5 cells(r=0.5, p<0.001), however, 18 of 57(32%) patients showed marked discrepancy of thyroid stimulating antibody activity between in hTSHR-CHO and FRTL-5 systems. Thyroid stimulating antibody activity measured by hTSHR-CHO cells was significantly correlated with serum total T3, free T4 levels, and goiter size but not 99mTc-thyroid uptake. On the other hand, thyroid stimulating antibody activity measured by FRTL-5 cells was significantly correlated with goiter size and 99mTc-thyroid uptake but not thyroid hormone levels. The difference between function and goiter size with respect to thyroid stimulating antibody measurement in two cells system is, nevertheless, particularly evident in the free T4/goiter ratio in patients with high hTSHR-CHO and low FRTL-5 cell assay values. Conclusion: These findings suggest that thyroid stimulating antibodies in Graves disease are heterogeneous population in terms of responses to different origin of cells. Further, thyroid stimulating antibody activities measured by FRTL-5 cells tend to correlate better with goiter size and Tc-thyroid uptake, whereas thyroid stimulating antibody activities measured by hTSH-CHO cells correlate better with thyroid hormone levels.

- Clinical Significance of Routine Measurement of Serum Calcitonin in Korean Patients with Thyroid Nodules as a Screening test of Sporadic Thyroid Medullary Carcinoma.
- Young Kee Shong, Cheol Soo Choi, Hye Young Park, Bo Youn Cho
- J Korean Endocr Soc. 1996;11(1):11-17. Published online November 7, 2019
- 1,093 View
- 27 Download
-
 Abstract
Abstract
 PDF
PDF - Background
: It is not easy to diagnose sporadic medullary thyroid carcinoma(MTC) before surgery and this might lead the patient reoperation and/or lowered chance of definite cure. Methods : The prevalence of sporadic MTC in Korean was studied in patients with thyroid nodules. A prospective study of 1048 consecutive patients with thyroid nodules was performed. In all patients, measurements of basal serum calcitonin, thyroid hormones, TSH, anti-thyroglobulin antibody and anti-thyroperoxidase antibody were undertaken along with technetium-99m thyroid scintigraphy and fine needle aspiration cytology. In patients with elevated basal calcitonin levels, calcium stimulated calcitonin level was determined. Results: Two patient had markedly elevated calcitonin levels(over 3,200 pg/mL and 1,763 pg/ mL) and another one slightly elevated calcitoni#n(71.9 pg/mL). Fine needle aspiration cytology was suggestive of MTC in one and nodular hyperplasia in the other two. They underwent surgery and histological examination revealed MTC in those two with markedly elevated calcitonin levels. The patient with slightly elevated calcitonin, who was on the maintenance hemodialysis due to chronic renal failure, had nodular hyperplasia. Conclusion: MTC was found in 0.19% of patients with thyroid nodules, which was not different with the previously reported prevalence in Europe. Routine measurements of serum calcitonin might be of value to detect sporadic MTC; however, the cost-effectiveness of routine measurement of serum calcitonin is not clear, considering the relatively low prevalence of MTC in Koreans.

- A Study on the Urinary Iodine Excretion in Normal subjects and Patients with Thyroid disease.
- Seong Yeon Kim, Bo Youn Cho, Hong Kyu Lee, Seok In Lee, Woon Bae Kim, Hye Young Park, Chang Soon Koh
- J Korean Endocr Soc. 1995;10(4):386-394. Published online November 7, 2019
- 1,344 View
- 69 Download
-
 Abstract
Abstract
 PDF
PDF - An adequate supply of dietary iodine is essential for the synthesis of the thyroid hormons. The measurement of dietary iodine intake is important for the clinical assessment of thyroid disease, especially in areas where iodine intake is excessive or deficient.To evaluate dietary iodine intake in Korean and its effects on thyroid function, we measured urinary iodine excretion with morning urine by electrode method in 184 normal subjects, 96 postpartum women and 181 patients with thyroid disease from October 1994 to February 1995. The results were as follows;1) In normal control, the mean value of urinary iodine excretion was 3.8+-2.7mg/L (range 0.1-15.0mg/L). However, there was no sex and age differences in the urinary iodine excretion.2) In postpartum women, the urinary iodine excretion was 9.0+-10.8mg/L who were not taken high iodine diet(Miyok-Guk), the mean value was statistically higher than normal control(p<0.01) and significant increased the urinary iodine excretion after eating of high iodine diet(p<0.01).3) In volunteer, there were increase of urinary iodine excretion more than 10 folds after high iodine diet and medication.4) The urinary iodine excretion in patients with thyroid diseases was not different from normal control, and there were no significant differences of urinary iodine excretion among the patient groups. The urinary iodine excretion in the acute stage of patients with subactue thyroiditis or painless thyroiditis was significantly increased compared to the recovery stage. However, it was not significantly different from that of normal control.In conclusion, urinary iodine excretion in Korean population is very high comparing to the reported data in Western population but similar with Japanese. The urinary iodine excretion is significant increase( more than 10-folds of basal level) after high iodine diet or high iodine containing medication in postpartum women or healthy persons. As a clue of destruction induced thyrotoxicosis, the urinary iodine excretion measurement is not valid in area where iodine intake is excessive like Korea.

- Assay of Thyrotropin Receptor Antibodies with Recombinant Human Thyrotropin Receptor Expressed on Chinese Hamster Ovary Cells.
- Bo Youn Cho, Hong Kyu Lee, Chang Soon Koh, Jae Hoon Chung, Ka Hee Yi, Kyung Soo Ko, Won Bae Kim
- J Korean Endocr Soc. 1995;10(4):347-361. Published online November 7, 2019
- 1,168 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Thyroid stimulating antibody which results in the development of hyperthyroidism and goiter in Graves' patients used to be measured by using rat thyroid cells, FRTL-5. However, this assay has disadvantages: decreased sensitivity due to differences in species, and fastidious culture conditions for FRTL-5 cells. Thus, we recently created stably transfected Chinese hamster ovary(CHO) cells containing the human TSH receptor(hTSHR-CHO) and developed optimal conditions for the measurement of thyroid stimulating antibody using hTSHR-CHO cells. In this study, to evaluate the clinical relevance of thyroid stimulating antibody measurement using hTSHR-CHO cells, we measured thyroid stimulating antibody activities of IgGs from Graves' disease and other thyroid disease using hTSHR-CHO cells, and compared to those of thyroid stimulating antibody assays using FRTL-5 cells. 1) The cut off value of positive thyroid stimulating antibody activity measured in hTSHR-CHO cells was 145%(above the mean +2SD) which was lower than 165% in FRTL-5 cells. The intra-assay and inter-assay variances were 3.9% to 9.0% and 12.7% to 1.6%, respectively. 2) Thyroid stimulating antibody activity was detected in 90% of patients with untreated Graves' disease when patients initially presented. Further, in patients seen initially but already under therapy, 75% had positive values if they were hyperthyroid but only 43% had IgGs with activity if they were euthyroid. Patients in clinical remission after therapy showed positive values in 23% of cases. Only 2 of 25 patients with Hashimoto's thyroiditis showed weak thyroid stimulating antibody activity, none of 18 patients with nodular nontoxie goiter, 1 of 15 patients with primary myxedema, and 2 of 33 control patients with no thyroid disease. Thus, the detection frequency and specificity of the assay with hTSHR-CHO cells was excellent for this type bioassay.3) The detection frequency of thyroid stimulating antibody activity by hTSHR-CHO cells assay system(90%) was higher than that by FRTL-5 cells assay system(66%) in untreated Graves' patients. Those two activities were positively correlated with each other(r=0.52, p<0.001). However, some IgGs showed discrepancy of the thyroid stimulating antibody activity measured in hTSHR-CHO cells and in FRTL-5 cells; 56 of 87 patients were positive in both cells system, 8 of 87 were negative in both cells system, 1 of 87 was only positive in FRTL-5 cells and 22 of 87 were only positive in hTSHR-CHO cell system. Thus, 73%(22/30) of IgGs showing negative values of thyroid stimulating antibody activities in FRTL-5 cells were detected its activities in hTSHR-CHO cells system.In summary, thyroid stimulating antibody assay with hTSHR-CHO cells exhibited so excellent sensitivity and specificity that this technique should be used for clinical practice as well as basic research.

- Thyroid Stimulating Antibody Assay with Chinese Hamster Ovary Cells Expressing Human Thyroid Stimulating Hormone (TSH) Receptor; Optimization of Assay Condition.
- Bo Youn Cho, Hong Kyu Lee, Young Kee Shong, Chang Soon Koh, Ka Hee Yi, Yeon Sahng Oh, Won Bae Kim
- J Korean Endocr Soc. 1995;10(4):333-346. Published online November 7, 2019
- 1,065 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - We investigated the optimal condition of thyroid stimulating antibody(TSAb) assay using Chinese hamster ovary cells transfected with cDNA of human TSH receptor(TSHr-CHO) stably expressing functional TSH receptors. The extracellular cAMP responses of TSHr-CHO cells to the stimulation of bTSH or Graves' IgG were observed in three different incubation media. Stimulation indices of extracellular cAMP were higher when sucrose containing NaCl-free isotonic Hank's balanced salt solution(HBSS)(media A)was used as incubation media than those of NaCl-free hypotonic HBSS(media B) or those of NaCl containing isotonic HBSS(media C). The incubation of TSHr-CHO cells in media B caused marked increase in the basal cAMP level without concomittant fold-increase in the stimulated cAMP level at various doses of bTSH and Graves' IgG. Decreasing the stimulation indices of extracellular cAMP, use of media B failed to detect TSAb activities in two TSAb-positive Graves' IgG tested. In case of media C, extracellular cAMP responses are poor at 0.001 and 0.1U/L of bTSH and at all doses of Graves' IgG tested(0.5, 1, 5g/L). The incubation of TSHr-CHO cells in media B caused significant increase in the number of trypan blue-stained, nonviable cells(5.7+-1.5, 7.6+-1.9 and 8.5+-1.6% at 1, 2 and 3h of incubation, respectively; p<0.01) comparing to those incubated in media A or media C(about 2-3% in both media). Those decrease in the viability of TSHr-CHO cells when incubated in hypotonic incubation media may explain the decrease in the stimulation index of extracellular cAMP with the use of media B in contrast to the case of FRTL-5 cells. TSAb assay of 87 consecutive fresh Graves' patients with TSHr-CHO cells using media A detected TSAb activities in 90%(78 patients) of them, and moreover TSAb activities showed significant positive correlation with the pre-treatment serum T_3 and free T_4 levels of those patients. We conclude that TSAb assay with TSHr-CHO cells is a sensitive and physiologically relevant assay system to measure TSAb activities merely through measurements of extracellular cAMP provided that the cells are incubated in NaCl-free isotonic incubation media.

Review Article
- Prognosis and Treatment of Differentiated Thyroid Cancer.
- Bo Youn Cho
- J Korean Endocr Soc. 1995;10(4):313-328. Published online November 7, 2019
- 1,164 View
- 18 Download

Original Article
- Relationship between Blood Pressure and Insulin Level or Red Cell Membrane Na+ Transport in Acromegaly.
- Seong Yeon Kim, Hyun Kyu Kim, Kyung Soo Park, Bo Youn Cho, Hong Kyu Lee, Chang Soon Koh
- J Korean Endocr Soc. 1995;10(1):35-44. Published online November 6, 2019
- 1,092 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - To test the hypothesis that hyperinsulinemia and/or abnormalities of red cell membrane Na^+ transport are concerned in the pathogenesis of hypertension, we investigated the relationship between blood pressure, insulin level and red cell membrane Na^+ transport in patients with acromegaly which is frequently associated with hypertension, hyperinsulinemia and abnormalities of red cell membrane Na^+ transport.The results were as follows;1) BMI and both systolic and diastolic blood pressure were significantly higher in patients with acromegaly than in control subjects.2) Fasting glucose and insulin levels were higher, and both serum glucose and insulin responses after a 75g glucose load were significantly increased in patients with acromegaly as compared with control subjects.3) Vmax of Na^+-Li^+ countertransport were significantly higher in patients with acromegaly than in control subjects while red cell Na^+ concentration and Vmax of Na^+, K^+ ATPase were similar in the two groups.4) In multiple stepwise regression analysis, age was directly correlated with both systolic and diastolic blood pressure in acromegaly. On the other hand both insulin level and red cell membrane Na^+ transport showed little correlation with either systolic or diastolic pressure. 5) Prevalence of hypertension in acromegaly was 39%(9 out of 23) and only age except for blood pressure was significantly higher in hypertensive acromegalic patients than in normotensive acromegalic patients while GH level, insulin levels and red cell membrane Na^+ transport were similar in the two groupsThese results suggest that hyperinsulinemia or abnormalities of red cell membrane Na^+ transport are not causally related to hypertension in patients with acromegaly.


 KES
KES

 First
First Prev
Prev



